For Pharma Companies

Solving the Challenges of Product Reach and Patient Support
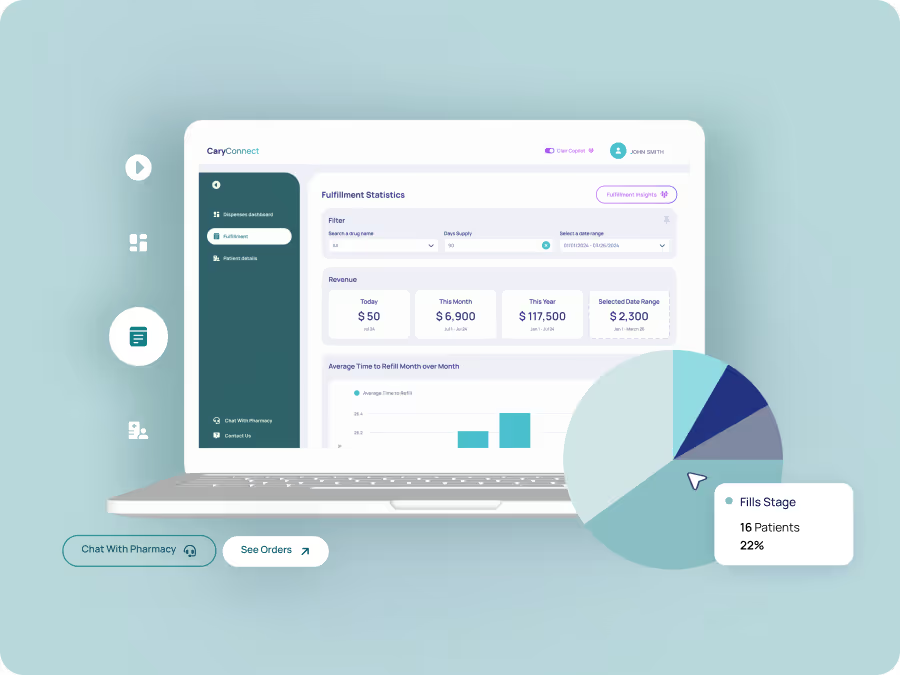
When pharma manufacturers can't see what's happening with prescription fulfillment and patient access, they can't evaluate how their products are performing or improve delivery.
CaryConnect provides insights and tools to spot bottlenecks, streamline distribution, and improve patient-provider engagement—ensuring continuous care.
Explore


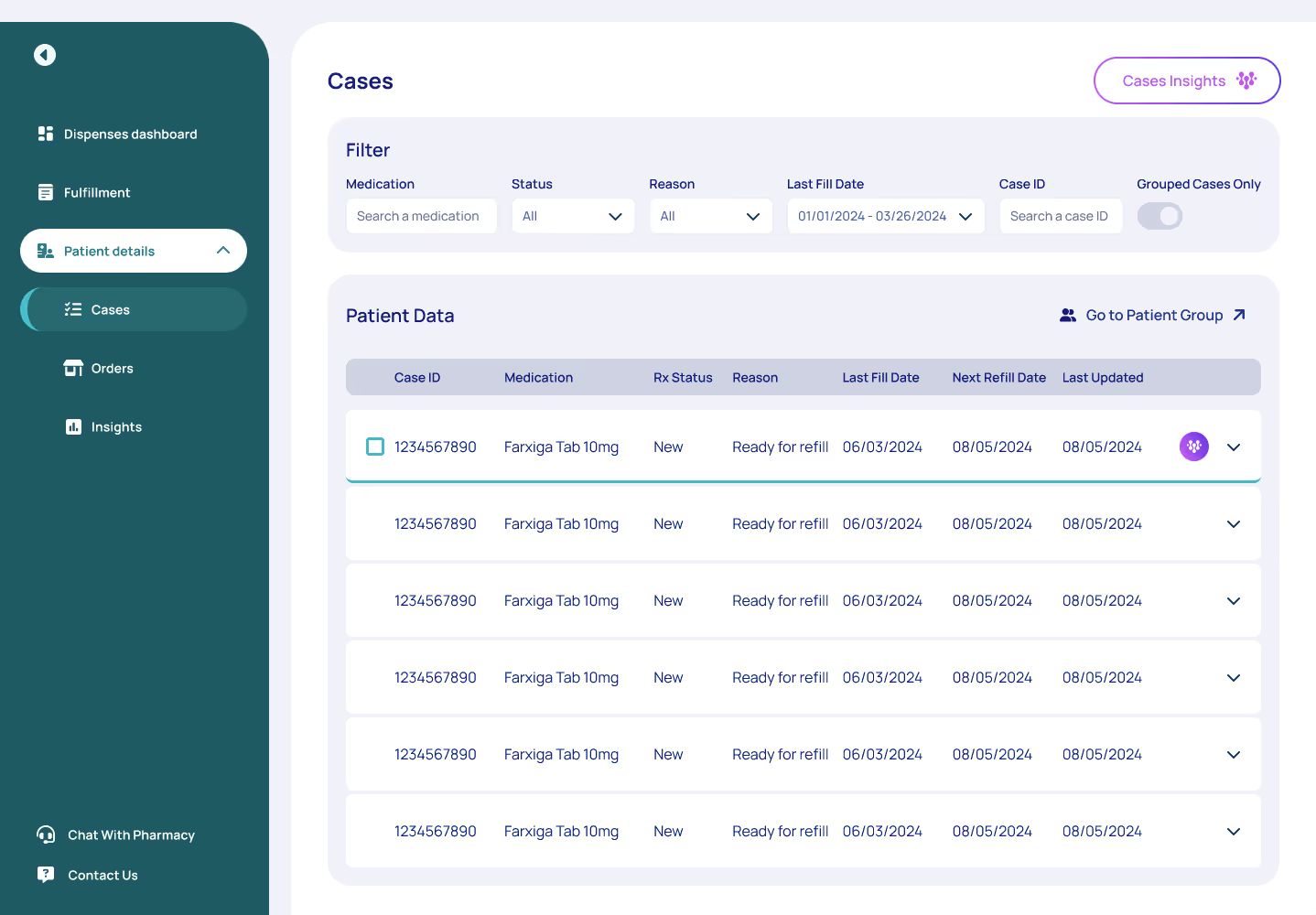
Real-Time Prescription Insights

Benefits Investigation Made Simple

Direct-to-Patient Health Experiences

Automated Patient Retention